Placement: Promote to Homepage

Nicole Davis
August 2, 2018
The human Y chromosome is, in many ways, a study in contrasts. For decades, scientists have struggled to dissect its evolution in part because it does not have a genetic partner (or homolog), as all of the other human chromosomes do. That solitary existence means the Y chromosome is subject to some unusual evolutionary pressures. For example, it does not swap genetic material with a homologous chromosome — a practice known as recombination that other chromosomes follow — along the lion’s share of its length. However, its lack of recombination presents a unique opportunity: Because so much of its own genetic material stays put, scientists can trace the history of individual human Y chromosomes much further back in time than other chromosomes — in fact, they can go as far back as the data will allow.
That is precisely the approach taken by a team of Whitehead Institute researchers, led by Whitehead Institute Director David Page, who is also a professor of biology at the Massachusetts Institute of Technology and a Howard Hughes Medical Institute investigator. Their work is published in the August 2nd online issue of the American Journal of Human Genetics. Page and his colleagues, including graduate student and first author Levi Teitz, set out to examine a series of regions on the Y chromosome called amplicons — vast stretches of DNA, from tens of thousands to millions of nucleotides in length, which are present in two or more copies per chromosome. While the DNA contained in amplicons is often highly repetitive, it also houses biologically important genes. Although the precise functions of many of these genes remains to be determined, some have been found to play important roles in the development of sperm cells and testicular cancer. However, the amplicons vary drastically among species, so scientists cannot look to other organisms such as mice or chimpanzees to help reconstruct their past.
Page’s team zeroed in on these amplicons. Specifically, they looked at how the number of amplicon copies varies from one person’s Y chromosome to another. The researchers developed sophisticated computational tools to analyze DNA sequencing data collected from more than 1,200 males as part of the 1000 Genomes Project. What they discovered was quite surprising. Although the amplicons are quite variable, they found that overall, the configuration of amplicon copies on the Y chromosome has been painstakingly maintained over the last 300,000 years of human evolution. That means that despite the high level of mutation the chromosome experiences, evolutionary forces work to counteract this change and preserve its ancestral structure.
More work is needed to determine which aspects of the amplicons’ structure are important for chromosome biology, and in turn proper male development and fertility. However, the efforts of Teitz, Page, and their colleagues shed new light on the unusual tricks the solo chromosome uses to maintain its genomic integrity.
This research is supported by the National Institutes of Health and the Howard Hughes Medical Institute.
Written by Nicole Davis
****
David Page’s primary affiliation is with Whitehead Institute for Biomedical Research, where his laboratory is located and all his research is conducted. He is also a Howard Hughes Medical Institute Investigator and a Professor of Biology at the Massachusetts Institute of Technology.
****
Full citation:
“Selection Has Countered High Mutability to Preserve the Ancestral Copy Number of Y Chromosome Amplicons in Diverse Human Lineages”
American Journal of Human Genetics, online August 2, 2018.
Levi S. Teitz (1,2), Tatyana Pyntikova (1), Helen Skaletsky (1,3), and David C. Page (1,2,3).
1. Whitehead Institute, Cambridge, MA 02142, USA
2. Department of Biology, Massachusetts Institute of Technology, Cambridge, MA 02142, USA
3. Howard Hughes Medical Institute, Whitehead Institute, Cambridge, MA 02142, USA

School of Science
July 23, 2018
The School of Science announced that eight of its faculty members have been appointed to named professorships. These positions afford the faculty members additional support to pursue their research and develop their careers.
Eliezer Calo, assistant professor in the Department of Biology, has been named the Irwin W. and Helen Sizer Career Development Professor. He focuses on the coordination of RNA metabolism using a combination of genetic, biochemical, and functional genomic approaches. The core of Calo’s research program is to understand how ribosome biogenesis is controlled by specific RNA binding proteins, particularly RNA helicases of the “DEAD box” family, and how disregulation of ribosome biogenesis contributes to various diseases, including cancer. He proposes initially to characterize the functions of specific genes of interest, including the DDX21 RNA helicase and the TCOF1 factor involved in RNA Pol I transcription and rRNA processing, using biochemical, molecular and genome-wide approaches in mouse, Xenopus and Zebrafish models.
Steven Flavell, assistant professor in the Department of Brain and Cognitive Sciences, has been named the Lister Brothers Career Development Professor. He uses Caenorhabditis elegans to examine how neuromodulators coordinate activity in neural circuits to generate locomotion behaviors linked to the feeding or satiety states of an animal. His long-term goal is to understand how neural circuits generate sustained behavioral states, and how physiological and environmental information is integrated into these circuits. Gaining a mechanistic understanding of how these circuits function will be essential to decipher the neural bases of sleep and mood disorders.
Pablo Jarillo-Herrero, the Cecil and Ida Green Professor of Physics, explores quantum transport in novel condensed-matter systems such as graphene, transition metal dichalcogenides and topological insulators. In recent work, he has demonstrated the presence of a bandgap in graphene-based van der Waals heterostructures, novel quantum spin Hall and photothermoelectric effects in graphene, as well as light-emitting diodes, photodetectors and solar cells in the atomically thin tungsten diselenide system. He has also made advances in characterizing and manipulating the properties of other ultrathin materials such as ultrathin graphite and molybdenum disulphide, which lack graphene’s ultrarelativistic properties, but possess other unusual electronic properties.
Becky Lamason, assistant professor in the Department of Biology, has been named the Robert A. Swanson (1969) Career Development Professor of Life Sciences. She investigates how intracellular bacterial pathogens hijack host cell processes to promote infection. In particular, she studies how Rickettsia parkeri and Listeria monocytogenes move through tissues via a process called cell-to-cell spread. She utilizes cellular, molecular, genetic, biochemical, and biophysical approaches to elucidate the mechanisms of spread in order to reveal key aspects of pathogenesis and host cell biology.
Rebecca Saxe, the inaugural John W. Jarve (1978) Professor in Brain and Cognitive Sciences, is best known for her discovery of a brain region that is specialized for “theory of mind,” people’s ability to think about the thoughts, beliefs, plans, hopes and emotions of other people. Saxe continues to study this region and its role in social cognition, and is exploring the theory-of-mind system as a promising candidate for understanding the biological basis of autism. She also studies brain development in human babies, including her own.
Omer Yilmaz, assistant professor in the Department of Biology, has been named the Eisen and Chang Career Development Professor. He studies how the adult intestine is maintained by stem cells that require a cellular neighborhood, or niche, consisting in part of Paneth cells. Specifically, he investigates the molecular mechanisms of how intestinal stem cells and their Paneth cell niche respond to diverse diets to coordinate intestinal regeneration with organismal physiology and its impact on the formation and growth of intestinal cancers. By better understanding how intestinal stem cells adapt to diverse diets, he hopes to identify and develop new strategies that prevent and reduce the growth of cancers involving the intestinal tract that includes the small intestine, colon, and rectum.
Yufei Zhao, assistant professor in the Department of Mathematics, has been named the Class of 1956 Career Development Professor. He has made significant contributions in combinatorics with applications to computer science. Recently, Zhao and three undergraduates solved an open problem concerning the number of independent sets in an irregular graph, a conjecture first proposed in 2001. Understanding the number of independent sets — subsets of vertices where no two vertices are adjacent — is important to solving many other combinatorial problems. In other research accomplishments, Zhao co-authored a proof with Jacob Fox and David Conlon that contributed to a better understanding of the celebrated Green-Tao theorem that states prime numbers contain arbitrarily long arithmetic progressions. Their work improves our understanding of pseudorandom structures — non-random objects with random-like properties — and has other applications in mathematics and computer science.
Martin Zwierlein, the inaugural Thomas A. Frank (1977) Professor of Physics, studies ultracold gases of atoms and molecules. These gases host novel states of matter and serve as pristine model systems for other systems in nature, such as neutron stars or high-temperature superconductors. In contrast to bulk materials, in experiments with cold gases one can freely tune the interaction between atoms and make it as strong as quantum mechanics allows. This enabled the observation of a novel robust form of superfluidity: Scaled to the density of electrons in solids, superfluidity would in fact occur far above room temperature. Under a novel quantum gas microscope with single-atom resolution, the team recently studied charge and spin correlations and transport in a Fermi-Hubbard lattice gas. This system is believed to hold the key to high-temperature superconductivity in cuprate materials. Using ultracold molecules, Zwierlein’s group also demonstrated coherence times on the order of seconds, spurring hopes for the future use of such molecules in quantum information applications.

Graduate student Julie Monda has spent five years investigating two divergent aspects of cell division, revealing some unexpected results and new research questions.
Raleigh McElvery
July 23, 2018
To sixth year graduate student Julie Monda, dividing cells are among the most beautiful things she’s ever seen. Watching the tiny, delicate spheres split into identical versions of themselves also provides her with a visual readout for her experiments — will the process continue if she removes a certain piece of a certain protein? Will the genetic material still distribute equally between the two cells? Which molecules are crucial for cell division, and how are they regulated?
Our cells are constantly dividing in order to grow and repair themselves, although some (like skin cells) do so more often than others, say, in the brain. This process, known as mitosis, is the primary focus of Iain Cheeseman’s lab, situated in the Whitehead Institute for Biomedical Research. Most of the research in the Cheeseman lab involves the kinetochore, a group of proteins located on the chromosome where the arms join. During mitosis, long, fibrous structures, known as microtubules, attach to the kinetochore to pull apart the duplicated chromosomes as the parent cell splits in half, ensuring each daughter cell receives an exact copy of the parent’s genetic blueprint.
Before she arrived at MIT Biology in the fall of 2012, Monda worked as a research technician at St. Jude Children’s Research Hospital in Memphis, Tennessee in the lab of Brenda Schulman PhD ’96 . As she recalls, she always “preferred performing hands-on research techniques at the lab bench over being in a classroom.” So she surprised even herself when she chose MIT’s graduate program in biology precisely because it requires all first-year students to take a full course load their fall semester before beginning lab rotations.
“That structure seemed useful given that I studied biochemistry as an undergraduate at the University of Tulsa, and the degree requirements were weighted more towards chemistry than biology,” she says. “Plus, when you’re only taking classes, you spend more time interacting with your classmates. It creates a close-knit community that extends throughout your entire graduate career and beyond.”
Monda ultimately selected the Cheeseman lab because it married her interests in biochemistry and cell biology.
“The research in this lab focuses on various elements of kinetochore function and cell division, but everyone is generally working on their own distinct questions,” she explains. “I knew I would have an area that was mine to explore. It’s both exciting and challenging because no one else is thinking about your projects to the extent that you are.”
Monda’s story is a tale of two projects: one focused on the interface between the kinetochore and the array of microtubules known as the mitotic “spindle,” and another project that ended up taking both her and the lab in a slightly new direction.
The first, concerning kinetochore-microtubule interactions, represented a collaboration with former lab technician Ian Whitney. For this endeavor, Monda investigated a protein complex called Ska1, found at the outer kinetochore.
The Ska1 complex is located where the kinetochore and microtubule meet. Ska1’s role, Monda explains, is to allow the kinetochores to remain attached to the spindle during chromosome segregation, even as the microtubules that compose the spindle begin to disassemble (as they must do).
“We wanted to know how the kinetochore hangs onto this polymer that is essentially falling apart,” Monda explains. “Long story short, we ended up defining specific surfaces within the Ska1 complex that are important for holding on to the microtubule as it shrinks, and — as we were surprised to note — also as it grows”
Although Ska1 only requires a single point of contact to bind a microtubule, Monda and Whitney pinpointed multiple surfaces on Ska1 that are required to allow it to remain associated with the microtubules as they disassemble and reassemble themselves.
While her Ska1 project was very much in line with the types of questions that the Cheeseman lab traditionally pursues, Monda also worked on another endeavor that “began as a side project and slowly evolved into a more full-time effort.” This project involves a motor protein called dynein, which helps to align the chromosomes and position the spindle during mitosis.
Dynein piqued Monda’s interest because of its role in mitosis, as well as its importance throughout the entire cell cycle. Motor proteins are molecules powered by the release of chemical energy that move along surfaces, sometimes transporting cargo, sometimes performing other essential tasks. Dynein is a motor protein that walks in one direction along microtubules, even when the microtubules latch onto the kinetochore to yank apart the chromosomes during mitosis.
But dynein doesn’t act alone. There are a number of additional proteins that also play a key role in coordinating its activity and localization. Monda is studying two of these accessory regulatory proteins, Nde1 and NdeL1, which bind to dynein and help promote some of its functions. She wanted to understand how Nde1 and NdeL1 interact with dynein to activate it. Although Nde1 and NdeL1 are nearly identical in function, Monda discovered that Nde1 (but not NdeL1) binds to another complex: the 26S proteasome.
The proteasome degrades proteins within the cell, influencing virtually all aspects of cellular function, including DNA synthesis and repair, transcription, translation, and cell signaling. Given its ubiquity, it has remained a point of interest among the scientific community for years. And yet, before Monda’s research, the interaction between Nde1 and the proteasome had apparently gone unnoticed. Researchers have long studied Nde1 in relation to dynein, but it’s possible that the interaction between Nde1 and the proteasome represents a new function for Nde1 unrelated to dynein regulation. In fact, Monda’s finding may have implications for understanding the development of the human brain.
“It’s clear that patients with mutations in Nde1 have much more severe neurodevelopmental defects than scientists would have predicted,” Monda says, “so it’s possible that this new interaction between Nde1 and the proteasome could help to explain why Nde1 is so important in the brain.”
Her most recent results have been published in Molecular Biology of the Cell.
“I’ve found some exciting results over the past few years,” Monda says, “and even though a lot of my research has gone in a direction that’s not strictly mitosis-related, Iain has been great about allowing me to follow the science wherever it leads. We want to know what these proteins are actually doing, both in terms of this new interaction and also more broadly within the cell.”
Monda intends to submit and defend her thesis this summer, and assume a postdoctoral position at the University California, San Diego in the fall. Although she’s been watching cells divide for years now, the process still retains its grandeur.
“Often times biologists investigate questions at scales where we can’t really see what we’re studying as we study it,” she says. “But having this visual readout makes it more tangible; I feel like I can better appreciate what exactly it is that I’m trying to understand, as well as the beauty and complexity of the processes that sustain life.”

Nicole Davis | Whitehead Institute
July 11, 2018
Cambridge, MA — Tackling unsolved problems is a cornerstone of scientific research, propelled by the power and promise of new technologies. Indeed, one of the shiniest tools in the biomedical toolkit these days is the genome editing system known as CRISPR/Cas9. Whitehead Institute Member David Sabatini and his colleagues pioneered the use of this tool as a foundation for large-scale genetic screens in human cells, turning up a treasure trove of new insights into cellular metabolism, in both normal cells and cancer cells.
When Naama Kanarek, a postdoc in Sabatini’s laboratory, pondered how to apply these state-of-the-art CRISPR/Cas9 screens to her own research, her thoughts turned to a classic cancer chemotherapy drug, methotrexate, which has been in clinical use for nearly seven decades. Often used to treat a form of pediatric leukemia, known as acute lymphoblastic leukemia (ALL), the drug, when deployed as part of a multifaceted treatment plan, can be highly effective. But its power comes at a cost. Because methotrexate can damage not only cancer cells but also healthy tissues, it must be administered with great care. For children who receive high doses of the drug, a mainstay of ALL treatment, that can mean several days spent in the hospital with rigorous clinical monitoring.
In other forms of cancer, methotrexate’s efficacy is more uncertain. For example, in pediatric osteosarcoma, only 65 percent of patients respond. Unfortunately, there is currently no way for doctors to pinpoint who will and who will not.
“From a scientific standpoint, methotrexate is quite special because it was the first metabolic drug to be developed, but much of its biology remains to be discovered — particularly what drives these different responses in patients,” Kanarek says. “So, this is really one of these old, classic questions that has been lingering in the field for some time. We thought we could learn something new.”
And they did. In the July 11 online issue of the journal Nature, Kanarek, Sabatini, and their colleagues report the findings of a CRISPR/Cas9 screen for factors involved in methotrexate sensitivity. The team’s work yielded a surprising set of discoveries that point to the breakdown of histidine — one of several amino acids used by the body to construct proteins — as a critical gatekeeper of cancer cells’ vulnerability to methotrexate. The researchers’ findings not only help illuminate the biology of a well-known cancer chemotherapy, but also suggest a simple dietary supplement that could help broaden its therapeutic window and reduce its toxicity.
“This study is an example of the power of modern genomic tools to shine a bright light on longstanding questions in human biology,” says senior author David Sabatini, a Member of Whitehead Institute, a professor of biology at Massachusetts Institute of Technology and investigator with the Howard Hughes Medical Institute (HHMI). “While cancer chemotherapies can be quite effective, their biological effects are often poorly understood. By laying bare their biology, we may be able to devise ways to utilize them more wisely.”
ATTACK THE CANCER, NOT THE PATIENT
The history of methotrexate stretches back to the 1940s, a time when strikingly little was known about the origins of cancer much less how best to treat it. The birth of methotrexate as a chemotherapeutic agent was sparked by the astute observations of Sidney Farber, a pediatric pathologist at Boston Children’s Hospital who cared for children with a variety of maladies, including ALL. In the course of caring for patients with ALL, Farber recognized that cancer cells depended on the nutrient folic acid for their own proliferation. That gave him the idea of using folate antagonists to treat ALL. Methotrexate was developed in 1949 precisely for this purpose and was subsequently shown to induce remission in children with ALL. Fast forward to today, and the drug has evolved into a significant tool in oncologists’ toolkit.
“Methotrexate is a major part of the backbone of chemotherapy treatment across many human cancers,” says Loren Walensky, a pediatric hematologist/oncologist at the Dana-Farber Cancer Institute who is not a study co-author but served as an early adviser on the project and will also play a deeper role in planning future follow-up studies. “It is also used outside of the cancer field for the treatment of several autoimmune diseases.”
He added, “But as with all chemotherapy, the critical issue is how to best use it to inflict maximal damage on the cancer without irreparably harming the patient.”
| Kanarek explains how new genetic tools are allowing insights into the sensitivity of cancer cells to methotrexate. |
The basic mechanics of methotrexate are fairly well known. The drug inhibits dihydrofolate reductase (DHFR), an enzyme that generates the functional form of folate, known as tetrahydrofolate (THF). THF is essential for preparing the raw materials needed to make nucleic acids, such as DNA, which carries cells’ genetic information, and RNA, a close chemical relative involved in making proteins. “Proliferating cells must duplicate their DNA, so they need a lot of THF,” Kanarek explains. “But even cells that are not dividing need to make RNA, and that requires THF, too.”
The results of Kanarek’s CRISPR/Cas9 screen now bring greater clarity to this molecular picture. She and her colleagues uncovered another enzyme, called FTCD, which is involved in the breakdown of histidine. Interestingly, FTCD also requires THF for its function — though not nearly as much as the main target of methotrexate, DHFR. Despite the differential demands of the two enzymes, they both draw from the same, shared pool of THF.
“Under normal conditions, this pool is sufficiently full, so there is no competition for resources, even in rapidly dividing cells,” Kanarek says.
But when the amount of THF becomes limiting — as it does in cells that are treated with methotrexate — the story is quite different, the Whitehead Institute team discovered. In that case, the activity of FTCD poses serious problems, because there isn’t enough THF in the pool to support both cell proliferation and histidine breakdown. When that happens, the cells die.
That got Kanarek thinking more about histidine: Could the nutrient provide a way to tinker with FTCD activity and, by virtue of the cancer cells’ own metabolism, make them more vulnerable to methotrexate?
To explore this question, the researchers used mouse models of leukemia, engineered by transplanting human leukemia cells under the skin of immunocompromised mice. A subset of the mice received injections of methotrexate together with histidine. This one-two punch, Kanarek hypothesized, should ramp up the function of FTCD and more rapidly drain the THF pool, thereby making the cells more sensitive to the cancer-killing effects of methotrexate.
That is precisely what the team observed. Notably, these experiments involved lower than normal doses of methotrexate, suggesting the cells had indeed been made more sensitive to the cancer drug. Moreover, the studies included a human leukemia cell line, called SEM, which harbors a specific genetic mutation that is associated with a particularly poor prognosis in patients — further underscoring the power of the histidine degradation pathway to weaken cells’ defenses.
Now, Kanarek and her colleagues are working to extend these initial findings with additional preclinical studies and, together with Walensky, determine how to best evaluate the potential benefits of histidine supplementation in cancer patients. Their ultimate goal: to pursue clinical trials that will assess histidine’s ability to improve the effectiveness of methotrexate in humans.
In addition to making cancer cells more vulnerable to methotrexate, the Whitehead Institute team’s research also holds promise for another therapeutic challenge: identifying which patients will or will not respond to the drug.
Two other enzymes cooperate with FTCD in breaking down histidine. The levels of one of the enzymes, known as HAL, appears to correlate with cells’ sensitivity to methotrexate: That is, cancer cells with high levels of HAL tend to be more sensitive to the drug. More work is needed to determine whether this correlation extends to a broader swath of patient samples and if it has predictive value in the clinic. Nevertheless, Kanarek and her colleagues are already beginning work on this front. Together with Abner Louissaint, Jr., a hematopathologist at Massachusetts General Hospital who also served as an early adviser on the Nature study, the Whitehead Institute team will launch a second clinical study to examine whether HAL levels can predict methotrexate response in patients with lymphoma.
“Being able to understand who is going to respond to methotrexate and who is not, and how to achieve a therapeutic benefit while mitigating the drug’s potential side effects, could have a profound impact on patient care,” Walensky says. “The insights from this study bring an entirely new dimension to our understanding of a decades-old and critically important cancer medicine. And as a physician and a scientist, that’s truly exciting.”
Written by Nicole Davis
* * *
David Sabatini’s primary affiliation is with Whitehead Institute for Biomedical Research, where his laboratory is located and all his research is conducted. He is also a Howard Hughes Medical Institute investigator and a professor of biology at Massachusetts Institute of Technology.
* * *
Full citation:
“Histidine catabolism is a major determinant of methotrexate sensitivity”
Nature, online on July 11, 2018.
Naama Kanarek (1,2,3,4), Heather R. Keys (1), Jason R. Cantor (1,2,3,4), Caroline A. Lewis (1), Sze Ham Chan (1), Tenzin Kunchok (1), Monther Abu-Remaileh (1,2,3,4), Elizaveta Freinkman (1), Lawrence D. Schweitzer (4), and David M. Sabatini (1,2,3,4).
- Whitehead Institute for Biomedical Research and Massachusetts Institute of Technology, Department of Biology, 455 main Street, Cambridge, Massachusetts 02142, USA
- Howard Hughes Medical Institute, Department of Biology, Massachusetts Institute of Technology, Cambridge, Massachusetts 02139, USA
- Koch Institute for Integrative Cancer Research and Massachusetts Institute of Technology, Department of Biology, 77 Massachusetts Avenue, Cambridge, Massachusetts 02139, USA
- Broad Institute of Harvard and Massachusetts Institute of Technology, 415 main Street, Cambridge, Massachusetts 02142, USA
MIT study finds synapses develop strength with calcium, maturation.
David Orenstein | Picower Institute for Learning and Memory
July 10, 2018
To work at all, the nervous system needs its cells, or neurons, to connect and converse in a language of electrical impulses and chemical neurotransmitters. For the brain to be able to learn and adapt, it needs the connections, called synapses, to be able to strengthen or weaken. A new study by neuroscientists at MIT’s Picower Institute for Learning and Memory helps to explain why strong synapses are stronger, and how they get that way.
By pinpointing the properties of synaptic strength and how they develop, the study could help scientists better understand how synapses might be made weaker or stronger. Deficiencies in synaptic development and change, or plasticity, have a role in many brain diseases such as autism or intellectual disability, says senior author Troy Littleton, the Menicon Professor of Neuroscience in MIT’s Department of Biology.
“The importance of our study is figuring out what are the molecular features of really strong synapses versus their weaker neighbors and how can we think about ways to convert really weak synapses to stronger ones,” Littleton says.
In the study, published in eLife, Littleton’s team used innovative imaging techniques in the model organism of the fruitfly Drosophila to focus on “active zones,” which are fundamental components of synapses. The scientists identified specific characteristics associated with a strong connection on both sides of the synapse.
The team, led by postdoc Yulia Akbergenova and graduate student Karen Cunningham, also studied how strong synapses and active zones grow, showing that those that have the longest to mature during a few critical days of development become the strongest.
Sources of strength
The team’s study began with a survey of active zones at a junction where a motor neuron links up a muscle. About 300 active zones were present at the neuromuscular junction, which gave the team a rich diversity of synapses to examine.
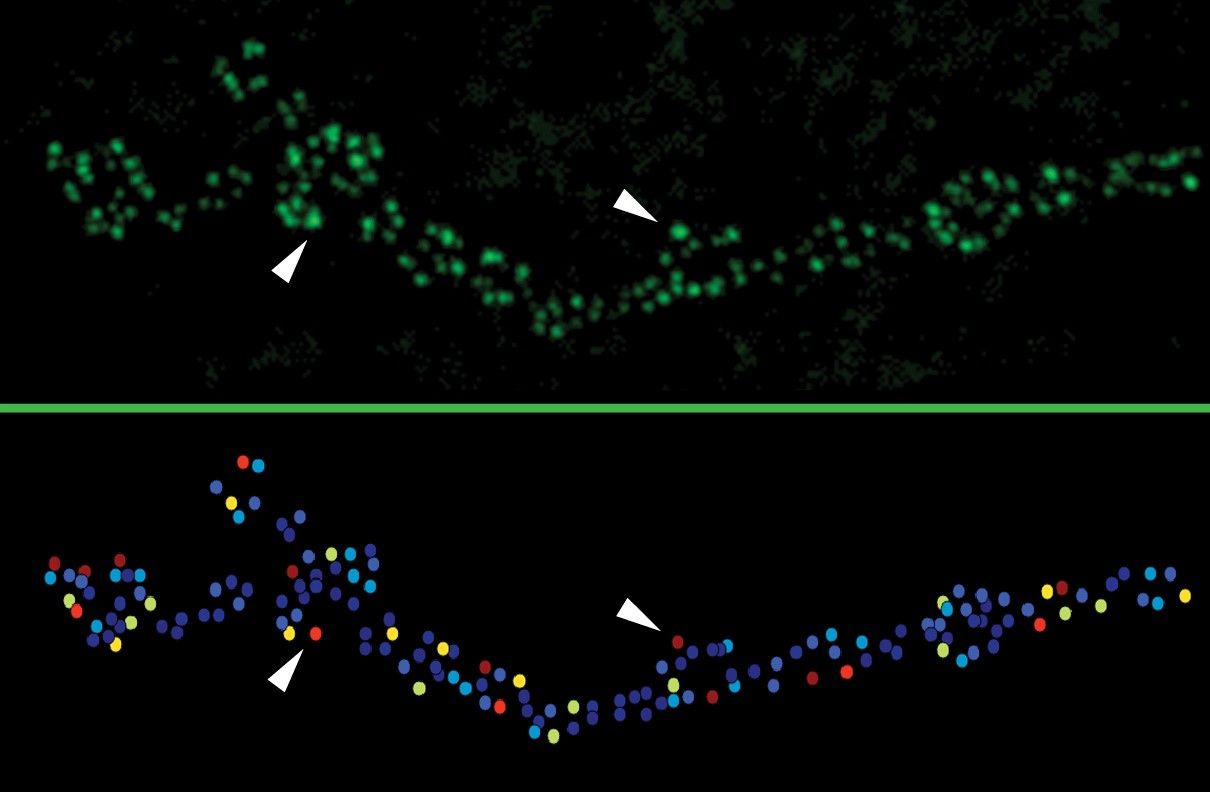
Typically, neuroscientists study neural connectivity by measuring the electrical currents in the postsynaptic neuron after activation of the presynaptic one, but such measures represent an accumulation of transmission from many active zones. In the new study, the team was able to directly visualize the activity of individual active zones with unprecedented resolution using “optical quantal imaging.”
“We optimized a genetically encoded calcium sensor to position it near active zones,” Akbergenova says. “This allows us to directly visualize activity at individual release sites. Now we can resolve synaptic transmission at the level of each individual release site.”
Across many flies, the team consistently found that only about 10 percent of the active zones at the junction were strong, as measured by a high likelihood that they would release the neurostransmitter glutamate when the presynaptic neuron was stimulated. About 70 percent of the active zones were much weaker, barely ever releasing glutamate given the same stimulation. Another 20 percent were inactive. The strongest active zones had release probabilities as much as 50 times greater than weak ones.
“The initial observation was that the synapse made by the exact same neuron are not of the same strength,” Littleton says. “So then the question became, what is it about an individual synapse that determines if it is strong or weak?”
The team ran several tests. In one experiment, for instance, they showed that it’s not their supply of synaptic vesicles, the containers that hold their cache of glutamate. When they stimulated the presynaptic neurons over and over, the strong ones retained their comparatively higher likelihood of release, even as their synaptic vesicle supply was intermixed with those from nearby active zones.
The presynaptic tests that showed a difference had to do with measuring the rate of calcium influx into the active zone and the number of channels through which that calcium reaches the active zone. Calcium ions stimulate the vesicles to fuse to the membrane of the presynaptic cell, allowing neurotransmitters to be released.
At strong synapses, active zones had a significantly greater influx of calcium ions through a notably higher abundance of calcium ion channels than weak synapse active zones did.
Stronger active zones also had more of a protein called Bruchpilot that helps to cluster calcium channels at synapses.
Meanwhile, on the postsynaptic side, when the scientists measured the presence and distribution of glutamate receptor subtypes they found a dramatic difference at strong synapses. In the typical weak synapse, GluRIIA and GluRIIB containing receptors were pretty much mixed together. But in strong synapses, the A subtype, which is more sensitive, crowded into the center while B was pushed out to the periphery, as if to maximize the receiving cell’s ability to pick up that robust signal.
Might through maturity
With evidence of what makes strong synapses strong, the scientists then sought to determine how they get that way and why there aren’t more of them. To do that, they studied each active zone from the beginning of development to several days afterward.
“This is the first time people have been able to follow a single active zone over many days of development from the time it is born in the early larvae through its maturation as the animal grows,” Littleton says.
They did this “intravital imaging” by briefly anesthetizing the larvae every day to check for changes in the active zones. Using engineered GluRIIA and GluRIIB receptor proteins that glow different colors they could tell when a strong synapse had formed by the characteristic concentration of A and marginalization of B.
One phenomenon they noticed was that active zone formation accelerated with each passing day of development. This turned out to be important because their main finding was that synapse strength was related to active zone age. As synapses matured over several days, they accumulated more calcium channels and BRP, meaning that they became stronger with maturity, but only a few had the chance to do it for several days.
The researchers also wanted to know whether activity affected the rate of maturation, as would be expected in a nervous system that must be responsive to an animal’s experience. By tinkering with different genes that modulate the degree of neuronal firing, they found that active zones indeed matured faster with more activity and slower when activity was reduced.
“These results provide a high resolution molecular and developmental understanding of several major factors underlying the extreme heterogeneity in release strength that exists across a population of active zones,” Cunningham says. “Since the cohort of proteins that make up the presynaptic active zone in flies is largely conserved in mammalian synapses, these results will provide valuable insight into how active zone release heterogeneity might arise in more complex neural systems.”
In addition to Littleton, Akbergenova, and Cunningham, the paper’s other authors are MIT postdoc Shirley Weiss-Sharabi and former MIT postdoc Yao Zhang.
The National Institutes of Health supported the research.

Initiative is building collections highlighting the contributions of female faculty.
Brigham Fay | MIT Libraries
July 6, 2018
A new MIT Libraries initiative aims to highlight MIT’s women faculty by acquiring, preserving, and making accessible their personal archives. The Institute Archives and Special Collections (IASC) launched the project last year with the generous support of Barbara Ostrom ’78 and Shirley Sontheimer.
The first year of the project has focused on reaching out to faculty who are ending the active phase of their careers. Four faculty members added their personal collections, comprising 234 boxes and 50 gigabytes of material. They are:
- Nancy Hopkins, the Amgen Inc. Professor of Biology Emerita, known for making zebrafish a widely used research tool and for bringing about an investigation that resulted in the landmark 1999 report on the status of women at MIT;
- Mary Potter, professor emerita in the Department of Brain and Cognitive Sciences, former chair of the MIT faculty, and member of the Committee of Women Faculty in the School of Science, whose research and teaching focused on experimental methods to study human cognition;
- Mary Rowe, adjunct professor at the MIT Sloan School of Management, special assistant to the president, and ombudsperson, a conflict resolution specialist whose work led to MIT having one of the nation’s first anti-harassment policies; and
- Sheila Widnall ’60, SM ’61, ScD ’64, Institute Professor and professor of aeronautics and astronautics, the first woman to serve as secretary of the Air Force, and the first woman to lead an entire branch of the U.S. military.
A donation of the papers of Mildred Dresselhaus, late Institute Professor emerita of electrical engineering and computer science and physics, is also forthcoming. Dresselhaus, whose work paved the way for much of today’s carbon-based nanotechnology, was also known for promoting opportunities for women in science and engineering. Discussions with additional faculty are also underway.
“We are honored to be stewards of these personal archives that have been given to MIT,” says Liz Andrews, project archivist. “We’re committed to preserving and making accessible these unique materials so they can be shared with the world into the future.”
Acquisitions of MIT administrative records provide additional context to the personal archives and a broader view on issues of gender equity and the challenges faced by women in academia. In the next phase of the project, archivists will continue to manage donations, prepare collections for use, and enlarge this core group by reaching out to female faculty who were tenured in the 1960s, ’70s, and ’80s.
Ultimately, the collections will provide not only rich resources for researchers, journalists, teachers, and students, but also, as Sontheimer says, inspiration for generations of women to come. “I’m hoping the project will encourage more women to become engaged in science, technology, and engineering,” she says.
Researchers identify the amino acid aspartate as a metabolic limitation in certain cancers.
Raleigh McElvery | Department of Biology
June 29, 2018
Remove tumor cells from a living organism and place them in a dish, and they will multiply even faster than before. The mystery of why this is has long stumped cancer researchers, though many have simply focused on the mutations and chains of molecular reactions that could prompt such a disparity. Now, a group of MIT researchers suggests that the growth limitations in live organisms may stem from a different source: the cell’s environment. More specifically, they found that the amino acid aspartate serves as a key nutrient needed for the “proliferation” or rapid duplication of cancer cells when oxygen is not freely available.
The biologists took cancer cells from various tissue types and engineered them to convert another, more abundant substrate into aspartate using the gene encoding an enzyme from guinea pigs. This had no effect on the cells sitting in a dish, but the same cells implanted into mice engendered tumors that grew faster than ever before. The researchers had increased the cells’ aspartate supply, and in doing so successfully sped up proliferation in a living entity.
“There hasn’t been a lot of thought into what slows tumor growth in terms of the cellular environment, including the sort of food cancer cells need,” says Matthew Vander Heiden, associate professor of biology, associate director of the Koch Institute for Integrative Cancer Research, and senior author of the study. “For instance, if you’re trying to get to a given destination and I want to slow you down, my best bet is to set up a roadblock at a place on your route where you’d experience a slow-down anyways, like a long traffic light. That’s essentially what we’re interested in here — understanding what nutrients the cell is already lacking that put the brakes on proliferation, and then further limiting those nutrients to inhibit growth even more.”
Lucas Sullivan, a postdoc in Vander Heiden’s lab, is the lead author of the study, which appeared in Nature Cell Biology on June 25.
Building the case for aspartate
Isolating a single factor that could impact tumor growth within an organism is tricky business. One potential candidate came to Sullivan via a paper he co-authored with graduate student Dan Gui in 2015, which asked a somewhat controversial question: Why is it that cells need to consume oxygen through cellular respiration in order to proliferate?
It’s a rather counter-intuitive question, because some scientific literature suggests just the opposite: Cancer cells in an organism (“in vivo”) do not enjoy the same access to oxygen as they would in a dish, and therefore don’t depend on oxygen to produce enough energy to divide. Instead, they switch to a different process, fermentation, that doesn’t require oxygen. But Sullivan and Gui noted that cancer cells do rely on oxygen for another reason: to produce aspartate as a byproduct.
Aspartate, they soon confirmed, does, in fact, play a crucial role in controlling the rate of cancer cell proliferation. In another study one year later, Sullivan and Gui noted that the antidiabetic drug metformin, known to inhibit mitochondria, slowed tumor growth and decreased aspartate levels in cells in vivo. Since mitochondria are key to cellular respiration, Sullivan reasoned that blocking their function in an already oxygen-constrained environment (the tumor) might make cancer cells vulnerable to further suppression of respiration — and aspartate — explaining why metformin seems to have such a strong effect on tumor growth.
Despite being potentially required for certain amino acids and the synthesis of all four DNA nucleotides, aspartate is already hard to come by, even in oxygen-rich environments. It’s among the lowest concentration amino acids in our blood, and has no way to enter our cells unless a rare protein transporter is present. Precisely why aspartate import is so inefficient remains an evolutionary mystery; one possibility is that its scarcity serves as a “failsafe,” preventing cells from multiplying until they have all the resources to properly do so.
Regardless, the easiest way for cells to get aspartate is not to import it from outside, but rather to make it directly inside, breaking down another amino acid called asparagine to generate it. However, there are very few known mammals that have an enzyme capable of producing aspartate from asparagine — among them, the guinea pig.
Channeling the guinea pig
In the 1950s, a researcher named John Kidd made an accidental discovery. He injected cancer-ridden rats with sera from various animals — rabbits, horses, guinea pigs, and the like — and discovered that guinea pig serum alone shrunk the rats’ tumors. It wasn’t until years later that scientists learned it was an enzyme in the guinea pig blood called guinea pig asparaginase 1 (gpASNase1) that was responsible for this antitumorigenic effect. Today, we know about a host of simpler organisms with similar enzymes, including bacteria and zebrafish. In fact, bacterial asparaginase is approved as a medicine to treat acute lymphocytic leukemia.
Because guinea pigs are mammals and thus have similar metabolisms to our own, the MIT researchers decided to use gpASNase1 to increase aspartate levels in tumors in four different tumor types and ask whether the tumors would grow faster. This was the case for three of the four types: The colon cancer cells, osteosarcoma cells, and mouse pancreatic cancer cells divided more rapidly than before, but the human pancreatic cancer cells continued to proliferate at their normal pace.
“This is a relatively small sample, but you could take this to mean that not every cell in the body is as sensitive to loss of aspartate production as others,” Sullivan says. “Acquiring aspartate may be a metabolic limitation for only a subset of cancers, since aspartate can be produced via a number of different pathways, not just through asparagine conversion.”
When the researchers tried to slow tumor growth using the antidiabetic metformin, the cells expressing gpASNase1 remained unaffected — confirming Sullivan’s prior suspicion that metformin slows tumor growth specifically by impeding cellular respiration and suppressing aspartate production.
“Our initial finding connecting metformin and proliferation was very serendipitous,” he says, “but these most recent results are a clear proof of concept. They show that decreasing aspartate levels also decreases tumor growth, at least in some tumors. The next step is to determine if there are other ways to more intentionally target aspartate synthesis in certain tissues and improve our current therapeutic approaches.”
Although the efficacy of using metformin to treat cancer remains controversial, these findings indicate that one means to target tumors would be to prevent them from accessing or producing nutrients like aspartate to make new cells.
“Although there are many limitations to cancer cell proliferation, which metabolites become limiting for tumor growth has been poorly understood,” says Kivanc Birsoy, the Chapman-Perelman Assistant Professor at Rockefeller University. “This study identifies aspartate as one such limiting metabolite, and suggests that its availability could be targeted for anti-cancer therapies.”
Birsoy is a former postdoc in professor of biology David Sabatini’s lab, who authored a paper published in the same issue of Nature Cell Biology, identifying aspartate as a major growth limitation in oxygen-deprived tumors.
“These companion papers demonstrate that some tumors in vivo are really limited by the chemical processes that require oxygen to get the aspartate they need to grow, which can affect their sensitivity to drugs like metformin,” Vander Heiden says. “We’re beginning to realize that understanding which cancer patients will respond to which treatments may be determined by factors besides genetic mutations. To really get the full picture, we need to take into account where the tumor is located, its nutrient availability, and the environment in which it lives.”
The research was funded by an NIH Pathway to Independence Award, the American Cancer Society, Ludwig Center for Molecular Oncology Fund, the National Science Foundation, a National Institutes of Health Ruth Kirschstein Fellowship, Alex’s Lemonade Stand Undergraduate Research Fellowship, Damon Runyon Cancer Research Foundation, Howard Hughes Medical Institute Faculty Scholar Award, Stand Up to Cancer, Lustgarten Foundation, Ludwig Center at MIT, the National Institutes of Health, and the Koch Institute’s Center for Precision Cancer Medicine.

Three MIT faculty members selected for funding from the G. Harold and Leila Y. Mathers Foundation.
Danielle Randall | Department of Chemistry
June 27, 2018
Research proposals from Laurie Boyer, associate professor of biology; Matt Shoulders, the Whitehead Career Development Associate Professor of Chemistry; and Feng Zhang, associate professor in the departments of Brain and Cognitive Sciences and Biological Engineering, Patricia and James Poitras ’63 Professor in Neuroscience, investigator at the McGovern Institute for Brain Research, and core member of the Broad Institute, have recently been selected for funding by the G. Harold and Leila Y. Mathers Foundation. These three grants from the Mathers Foundation will enable, over the next three years, key projects in the researchers’ respective labs.
Regenerative medicine holds great promise for treating heart failure, but that promise is unrealized, in part, due to a lack of sufficient understanding of heart development at the mechanistic level. Boyer’s research aims to achieve a deep, mechanistic understanding of the gene control switches that coordinate normal heart development. She then aims to leverage this knowledge and design effective strategies for rewiring faulty circuits in aging and disease.
“We are very grateful to receive support and recognition of our work from the Mathers Foundation,” said Boyer. “This award will allow us to build upon our prior work and to embark upon high risk projects that could ultimately change how we think about treating diseases resulting from faulty wiring of gene expression programs.”
Shoulders’ goal, with this support from the Mathers Foundation, is to elucidate underlying causes of osteoarthritis. There is currently no cure for osteoarthritis, which is perhaps the most common aging-related disease and is characterized by a progressive deterioration of joint cartilage culminating in inflammation, debilitating pain, and joint dysfunction. The Shoulders Group aims to test a new model for osteoarthritis — specifically, the concept that a collapse of proteostasis in aging cartilage cells creates an unrecoverable cartilage repair defect, thus initiating a self-amplifying, destructive feedback loop leading to pathology. Proteostasis collapse in aging cells is a well-known, disease-causing phenomenon that has previously been considered primarily in the context of neurodegenerative disorders. If correct, the proteostasis collapse model for osteoarthritis could one day lead to a novel class of therapeutic options for the disease.
“We are delighted to receive this generous support from the Mathers Foundation, which makes it possible for us to pursue an outside-the-box, high-risk/high-impact idea regarding the origins of osteoarthritis,” said Shoulders. “The research we are now able to pursue will not only provide fundamental, molecular-level insights into joint function, but also could change how we think about this widespread disease.”
Many genetic diseases are caused by the change of just a single base of DNA. Zhang is a leader in the field of genome editing, and he and his team have developed an array of tools based on the microbial immune CRISPR-Cas systems that can manipulate DNA and RNA in human cells. Together, these tools are changing the way molecular biology research is conducted, and they hold immense potential as therapeutic agents to correct thousands of genetic diseases. Now, with the support of the Mathers Foundation, Zhang is working to realize this potential by developing a CRISPR-based therapeutic that works at the level of RNA and offers a safe, effective route to treating a range of diseases, including diseases of the brain and central nervous system, which are difficult to treat with existing gene therapies.
“The generous support from the Mathers Foundation allows us the freedom to explore this exciting new direction for CRISPR-based technologies,” Zhang stated.
Known for their generosity and philanthropy, G. Harold and Leila Y. Mathers created their foundation with the goal of distributing their wealth among sustainable, charitable causes, with a particular interest in basic scientific research. The Mathers Foundation, whose ongoing mission is to advance knowledge in the life sciences by sponsoring scientific research and applying learnings and discoveries to benefit mankind, has issued grants since 1982.

Mechanism-based cancer prevention is poised to further decrease the numbers of U.S. cancer deaths, says MIT professor emerita.
Anne Trafton | MIT News Office
June 25, 2018
Great progress has already been made in reducing the cancer death toll through prevention, according to a new article in the June 25 issue of Genes and Development by MIT Professor Emerita Nancy Hopkins and colleagues from the Broad Institute, Fox Chase Cancer Center, University of Texas M.D. Anderson Cancer Center, and Oxford University. The potential for further reduction is great for two reasons, these researchers say: If these approaches can be more widely applied, in principle about half of current U.S. cancer deaths could be prevented over the next two to three decades; and new discoveries about how cancer develops could help scientists develop even better prevention and screening methods. MIT News spoke with Hopkins, the Amgen Inc. Professor of Biology Emerita, about why this is an exciting time for cancer research.
Q: What does your new article reveal about the impact of cancer prevention and early detection?
A: We’ve described how researchers are integrating the dramatic advances in understanding the molecular biology of cancer to explain long-known facts about how lifestyle choices and factors in the environment affect how cancers arise, and how they progress to become detectable tumors.
Prevention and early detection have already had a tremendous impact on reducing U.S. cancer death rates. In the cancer prevention community, it is well-known that about half of current U.S. cancer deaths could, in theory, be prevented over the next two to three decades simply by the full uptake of proven methods of cancer prevention. This important fact is not as well appreciated by the larger cancer research community. This is not a fault of the cancer researchers; it simply reflects the reality that after years of investment and growth, the field of cancer is very broad, with most people working in areas of specialty.
Given the difficulties in treating established cancers, preventing many cancers entirely would obviously produce a quantal leap in reducing U.S. cancer death rates. But in addition, we believe that recent progress in understanding the molecular mechanisms that underlie cancer, and new technologies associated with these advances, could also lead to novel approaches to preventing cancer, detecting it at earlier stages when treatment is often far more successful, or even intercepting the progression of incipient cancers before they develop into tumors.
Q: What interventions have had success preventing cancer, and what promising new approaches are on the horizon?
A: Spectacular examples of preventing cancers from arising in the first place (formally called “primary cancer prevention”) include (1) successful efforts that reduced smoking rates in the United States (from over 40 percent in the 1960s to about 15 percent today) and that have led to a decline in the incidence of lung cancer and a dozen or more other types of cancer caused by smoking; (2) vaccines for cancer-causing viruses, including hepatitis B virus (a cause of liver cancer) and papilloma viruses (the cause of cervical, head and neck, and several other cancers); (3) clean air and water acts and safer workplace laws in the United States that have prevented workers as well as the general population from exposure to high concentrations of certain industrial chemicals known to cause cancer; (4) the development of drugs to cure hepatitis C infection, which are expected to prevent the development of liver cancer in the future; (5) campaigns such as the one in Australia to prevent skin cancers (particularly melanoma) by behavioral changes related to sun exposure.
As for promising new approaches to primary cancer prevention, the fuller uptake of proven methods of prevention is obviously one way to ensure a dramatic decrease in U.S. cancer death rates in the next two to three decades. This would require a greater investment in public health measures. As our article outlines, we are only now coming to understand the mechanisms by which factors such as obesity, inflammation, and some lifestyle choices synergize with long-appreciated risk factors to promote cancer. Based on this improved understanding, prevention could also be aided by research into new drugs, for example to prevent nicotine addiction or to intercept cancer progression by targeting inflammation. Exciting, too, is the possibility that DNA sequencing of cancer genomes may help to identify additional external causes of cancers based on the “mutational signatures” they leave in our DNA after exposures. If so, these agents may prove to be removable or avoidable in future.
We also discuss a second type of intervention to prevent cancer. This is screening, sometimes referred to as “secondary cancer prevention,” which can detect precancers and cancers at an early enough stage to remove them completely or treat them much more successfully. Spectacular successes to date include the Pap test that has greatly reduced deaths from cervical cancer in the United States and elsewhere; newer molecular tests focused on HPV-virus detection have proven similarly effective and are now replacing traditional Pap tests which require expert pathologic interpretations, making screening more widely available. A second success is colonoscopy, which has been enormously successful at detecting precancerous polyps and early-stage colon cancers that can be removed through the endoscope, or detected earlier when they’re more likely to be responsive to treatment. Additionally, other less-invasive methods of colon cancer screening are readily available and highly effective. Also successful has been mammography in combination with follow-up treatment. Along with greatly improved treatment, it is credited with contributing to the declining death rate from breast cancer.
Q: What types of new screening methods do you believe could help to further improve early detection of cancer?
A: Many of the most successful screening methods are for cancers that develop on body surfaces and hence can be detected by visual inspection. Imaging can be hugely successful for cancers that lie deeper in the body — breast for example — but imaging that becomes more and more sensitive can identify many abnormalities that may not be cancer at all. This can lead to costly and invasive testing of what are sometimes referred to as “incidentalomas.” Much needed are novel methods of screening that may combine imagining with other markers to make it possible to distinguish true cancers from noncancerous aberrations occurring in internal organs.
The holy grail of cancer screening would be blood tests to detect early-stage cancers, and many efforts are now directed to this goal. This is an extremely exciting time for the emergence of powerful molecular diagnostics that can help pinpoint very early-stage tumors. Some of these rely on relatively noninvasive methods, such as measurement of DNA signatures found in the blood. Widespread availability and demonstrated effectiveness of such methods would greatly enhance the field of secondary prevention, but there remain substantial challenges and it is not yet known if this approach will succeed. Also very exciting are methods being developed by bioengineers here at MIT and in other places to try to amplify other signals arising from tumors that may be difficult to detect otherwise and include, for example, completely noninvasive urine-based tests.
After decades of effort, cancer is gradually coming under control thanks to prevention and early detection, improvements in “conventional” cancer treatment (imaging, surgery, radiation, chemotherapy, and some adjuvant therapies), and novel approaches to treatment based on immunotherapy and more personalized drugs. But it is likely that for now, the full implementation of proven methods of prevention offers the most reliable approach to large-scale reduction of U.S. cancer deaths. Meanwhile, research into novel mechanism-based approaches to preventing the initiation and progression of cancer may one day prevent the majority of cancers from occurring in the first place.
