Research Area: Cell Biology
December 15, 2021

The clinically-trained cell biologist exploits the liver’s unique capacities in search of new medical applications.
Grace van Deelen | Department of Biology
December 15, 2021
Why is the liver the only human organ that can regenerate? How does it know when it’s been injured? What can our understanding of the liver contribute to regenerative medicine? These are just some of the questions that new assistant professor of biology Kristin Knouse and her lab members are asking in their research at the Koch Institute for Integrative Cancer Research. Knouse sat down to discuss why the liver is so unique, what lessons we might learn from the organ, and what its regeneration might teach us about cancer.
Q: Your lab is interested in questions about how body tissues sense and respond to damage. What is it about the liver that makes it a good tool to model those questions?
A: I’ve always felt that we, as scientists, have so much to gain from treasuring nature’s exceptions, because those exceptions can shine light onto a completely unknown area of biology and provide building blocks to confer such novelty to other systems. When it comes to organ regeneration in mammals, the liver is that exception. It is the only solid organ that can completely regenerate itself. You can damage or remove over 75 percent of the liver and the organ will completely regenerate in a matter of weeks. The liver therefore contains the instructions for how to regenerate a solid organ; however, we have yet to access and interpret those instructions. If we could fully understand how the liver is able to regenerate itself, perhaps one day we could coax other solid organs to do the same.
There are some things we already know about liver regeneration, such as when it begins, what genes are expressed, and how long it takes. However, we still don’t understand why the liver can regenerate but other organs cannot. Why is it that these fully differentiated liver cells — cells that have already assumed specialized roles in the liver — can re-enter the cell cycle and regenerate the organ? We don’t have a molecular explanation for this. Our lab is working to answer this fundamental question of cell and organ biology and apply our discoveries to unlock new approaches for regenerative medicine. In this regard, I don’t necessarily consider myself exclusively a liver biologist, but rather someone who is leveraging the liver to address this much broader biological problem.
Q: As an MD/PhD student, you conducted your graduate research in the lab of the late Professor Angelika Amon here at MIT. How did your work in her lab lead to an interest in studying the liver’s regenerative capacities?
A: What was incredible about being in Angelika’s lab was that she had an interest in almost everything and gave me tremendous independence in what I pursued. I began my graduate research in her lab with an interest in cell division, and I was doing experiments to observe how cells from different mammalian tissues divide. I was isolating cells from different mouse tissues and then studying them in culture. In doing that, I found that when the cells were isolated and grown in a dish they could not segregate their chromosomes properly, suggesting that the tissue environment was essential for accurate cell division. In order to further study and compare these two different contexts — cells in a tissue versus cells in culture — I was keen to study a tissue in which I could observe a lot of cells undergoing cell division at the same time.
So I thought back to my time in medical school, and I remembered that the liver has the ability to completely regenerate itself. With a single surgery to remove part of the liver, I could stimulate millions of cells to divide. I therefore began exploiting liver regeneration as a means of studying chromosome segregation in tissue. But as I continued to perform surgeries on mice and watch the liver rapidly regenerate itself, I couldn’t help but become absolutely fascinated by this exceptional biological process. It was that fascination with this incredibly unique but poorly understood phenomenon — alongside the realization that there was a huge, unmet medical need in the area of regeneration — that convinced me to dedicate my career to studying this.
Q: What kinds of clinical applications might a better understanding of organ regeneration lead to, and what role do you see your lab playing in that research?
A: The most proximal medical application for our work is to confer regenerative capacity to organs that are currently non-regenerative. As we begin to achieve a molecular understanding of how and why the liver can regenerate, we put ourselves in a powerful position to identify and surmount the barriers to regeneration in non-regenerative tissues, such as the heart and nervous system. By answering these complementary questions, we bring ourselves closer to the possibility that, one day, if someone has a heart attack or a spinal cord injury, we could deliver a therapy that stimulates the tissue to regenerate itself. I realize that may sound like a moonshot now, but I don’t think any problem is insurmountable so long as it can be broken down into a series of tractable questions.
Beyond regenerative medicine, I believe our work studying liver regeneration also has implications for cancer. At first glance this may seem counterintuitive, as rapid regrowth is the exact opposite of what we want cancer cells to do. However, the reality is that the majority of cancer-related deaths are attributable not to the rapidly proliferating cells that constitute primary tumors, but rather to the cells that disperse from the primary tumor and lie dormant for years before manifesting as metastatic disease and creating another tumor. These dormant cells evade most of the cancer therapies designed to target rapidly proliferating cells. If you think about it, these dormant cells are not unlike the liver: they are quiet for months, maybe years, and then suddenly awaken. I hope that as we start to understand more about the liver, we might learn how to target these dormant cancer cells, prevent metastatic disease, and thereby offer lasting cancer cures.
Eva Frederick | Whitehead Institute
December 2, 2021
Humans need oxygen molecules for a process called cellular respiration, which takes place in our cells’ mitochondria. Through a series of reactions called the electron transport chain, electrons are passed along in a sort of cellular relay race, allowing the cell to create ATP, the molecule that gives our cells energy to complete their vital functions.
At the end of this chain, two electrons remain, which are typically passed off to oxygen, the “terminal electron acceptor.” This completes the reaction and allows the process to continue with more electrons entering the electron transport chain.
In the past, however, scientists have noticed that cells are able to maintain some functions of the electron transport chain, even in the absence of oxygen. “This indicated that mitochondria could actually have partial function, even when oxygen is not the electron acceptor,” said Whitehead Institute postdoctoral researcher Jessica Spinelli. “We wanted to understand, how does this work? How are mitochondria capable of maintaining these electron inputs when oxygen is not the terminal electron acceptor?”
In a paper published December 2 in the journal Science, Whitehead Institute scientists and collaborators led by Spinelli have found the answer to these questions. Their research shows that when cells are deprived of oxygen, another molecule called fumarate can step in and serve as a terminal electron acceptor to enable mitochondrial function in this environment. The research, which was completed in the laboratory of former Whitehead Member David Sabatini, answers a long-standing mystery in the field of cellular metabolism, and could potentially inform research into diseases that cause low oxygen levels in tissues, including ischemia, diabetes and cancer.
A new runner in the cellular relay
The researchers began their investigation into how cells can maintain mitochondrial function without oxygen by using mass spectrometry to measure the quantities of molecules called metabolites that are produced through cellular respiration in both normal and low-oxygen conditions. When cells were deprived of oxygen, researchers noticed a high level of a molecule called succinate.
When you add electrons to oxygen at the end of the electron transport chain, it picks up two protons and becomes water. When you add electrons to fumarate, it becomes succinate. “This led us to think that maybe this accumulation of succinate that’s occurring could actually be caused by fumarate being used as an electron acceptor, and that this reaction could explain the maintenance of mitochondrial functions in hypoxia,” Spinelli said.
Usually, the fumarate-succinate reaction runs the other direction in cells — a protein complex called the SDH complex takes away electrons from succinate, leaving fumarate. For the opposite to happen, the SDH complex would need to be running in reverse. “Although the SDH complex is known to catalyze some fumarate reduction, it was thought that it was thermodynamically impossible for this SDH complex to undergo a net reversal,” Spinelli said. “Fumarate is used as an electron acceptor in lower eukaryotes, but they use a totally different enzyme and electron carrier, and mammals are not known to possess either of these.”
Through a series of assays, however, the researchers were able to ascertain that this complex was indeed running in reverse in cultured cells, largely due to accumulation of a molecule called ubiquinol, which the researchers observed to build up under low-oxygen conditions.
With their hypothesis confirmed, “We wanted to get back to our initial question and ask, does that net reversal of the SDH complex maintain mitochondrial functions which are happening when cells are exposed to hypoxia?” said Spinelli. “So, we knocked out SDH complex and then we demonstrated through a number of means that loss of both oxygen and fumarate as an electron acceptors was sufficient to [bring the electron transport chain to a halt].”
All this work was done in cultured cells, so the next step for Spinelli and collaborators was to study whether fumarate could serve as a terminal electron acceptor in mouse models.
When they tried this, the team uncovered something interesting: some, but not all, of the mice’s tissues were able to successfully reverse the activity of the SDH complex and perform mitochondrial functions using fumarate as a terminal electron acceptor.
“What was really cool to see is that there were three tissues — the kidney, the liver, and the brain — which on a bulk tissue scale, are operating the SDH complex in a backwards direction, even at physiological oxygen levels,” said Spinelli. In other words, even in normal conditions, these tissues were reducing both fumarate and oxygen to maintain their functions, and when deprived of oxygen, fumarate could take over as a terminal electron acceptor.
In contrast, tissues such as the heart and the skeletal muscle are able to perform minimal fumarate reduction without reversing the SDH complex, but not to the extent that they could effectively retain mitochondrial function when deprived of oxygen.
“We think there’s a lot of exciting work downstream of this to figure out how exactly this process is regulated differently in different tissues — and understanding in disease settings whether the SDH complex is operating in the net reverse direction,” Spinelli said.
In particular, Spinelli is interested in studying the behavior of the SDH complex in cancer cells.
“Certain regions of solid tumors have very low levels of oxygen, and certain regions have high levels of oxygen,” Spinelli said. “It’s interesting to think about how those cells are surviving in that microenvironment — are they using fumarate as an electron acceptor to enable cell survival?”
December 2, 2021
November 18, 2021
November 12, 2021
November 3, 2021
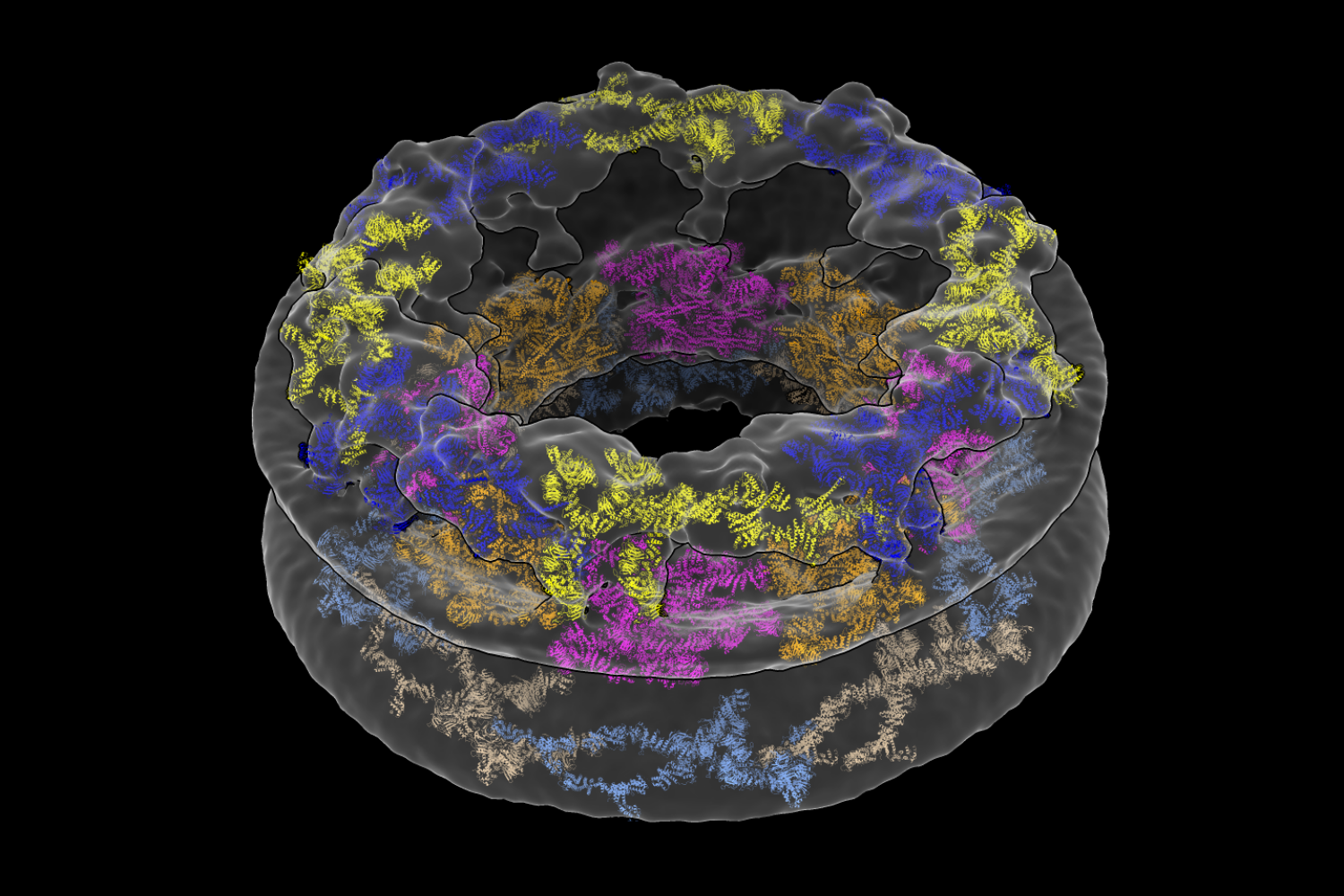
Researchers glean a more complete picture of a complex structure called the nuclear pore complex by studying it directly inside cells.
Raleigh McElvery | Department of Biology
October 13, 2021
Context matters. It’s true for many facets of life, including the tiny molecular machines that perform vital functions inside our cells.
Scientists often purify cellular components, such as proteins or organelles, in order to examine them individually. However, a new study published today in the journal Nature suggests that this practice can drastically alter the components in question.
The researchers devised a method to study a large, donut-shaped structure called the nuclear pore complex (NPC) directly inside cells. Their results revealed that the pore had larger dimensions than previously thought, emphasizing the importance of analyzing complex molecules in their native environments.
“We’ve shown that the cellular environment has a significant impact on large structures like the NPC, which was something we weren’t expecting when we started,” says Thomas Schwartz, the Boris Magasanik Professor of Biology at MIT and the study’s co-senior author. “Scientists have generally thought that large molecules are stable enough to maintain their fundamental properties both inside and outside a cell, but our findings turn that assumption on its head.”
In eukaryotes like humans and animals, most of a cell’s DNA is stored in a rounded structure called the nucleus. This organelle is shielded by the nuclear envelope, a protective barrier that separates the genetic material in the nucleus from the thick fluid filling the rest of the cell. But molecules still need a way to come in and out of the nucleus in order to facilitate important processes, including gene expression. That’s where the NPC comes in. Hundreds — sometimes thousands — of these pores are embedded in the nuclear envelope, creating gateways that allow certain molecules to pass.
The study’s first author, former MIT postdoc Anthony Schuller, compares NPCs to gates at a sports stadium. “If you want to access the game inside, you have to show your ticket and go through one of these gates,” he explains.
The NPC may be tiny by human standards, but it’s one of the largest structures in the cell. It’s comprised of roughly 500 proteins, which has made its structure challenging to parse. Traditionally, scientists have broken it up into individual components to study it piecemeal using a method called X-ray crystallography. According to Schwartz, the technology required to analyze the NPC in a more natural environment has only recently become available.
Together with researchers from the University of Zurich, Schuller and Schwartz employed two cutting-edge approaches to solve the pore’s structure: cryo-focused ion beam (cryo-FIB) milling and cryo-electron tomography (cryo-ET).
An entire cell is too thick to look at under an electron microscope. But the researchers sliced frozen colon cells into thin layers using the cryo-FIB equipment housed at MIT.nano’s Center for Automated Cryogenic Electron Microscopy and the Koch Institute for Integrative Cancer Research’s Peterson (1957) Nanotechnology Materials Core Facility. In doing so, the team captured cross-sections of the cells that included NPCs, rather than simply looking at the NPCs in isolation.
“The amazing thing about this approach is that we’ve barely manipulated the cell at all,” Schwartz says. “We haven’t perturbed the cell’s internal structure. That’s the revolution.”
What the researchers saw when they looked at their microscopy images was quite different from existing descriptions of the NPC. They were surprised to find that the innermost ring structure, which forms the pore’s central channel, is much wider than previously thought. When it’s left in its natural environment, the pore opens up to 57 nanometers — resulting in a 75 percent increase in volume compared to previous estimates. The team was also able to take a closer look at how the NPC’s various components work together to define the pore’s dimensions and overall architecture.
“We’ve shown that the cellular environment impacts NPC structure, but now we have to figure out how and why,” Schuller says. Not all proteins can be purified, he adds, so the combination of cryo-ET and cryo-FIB will also be useful for examining a variety of other cellular components. “This dual approach unlocks everything.”
“The paper nicely illustrates how technical advances, in this case cryo-electron tomography on cryo-focused ion beam milled human cells, provide a fresh picture of cellular structures,” says Wolfram Antonin, a professor of biochemistry at RWTH Aachen University in Germany who was not involved in the study. The fact that the diameter of the NPC’s central transport channel is larger than previously thought hints that the pore could have impressive structural flexibility. “That may be important for the cell to adapt to increased transport demands,” Antonin explains.
Next, Schuller and Schwartz hope to understand how the size of the pore affects which molecules can pass through. For instance, scientists only recently determined that the pore was big enough to allow intact viruses like HIV into the nucleus. The same principle applies to medical treatments: only appropriately-sized drugs with specific properties will be able to access the cell’s DNA.
Schwartz is especially curious to know whether all NPCs are created equal, or if their structure differs between species or cell types.
“We’ve always manipulated cells and taken the individual components out of their native context,” he says. “Now we know this method may have much bigger consequences than we thought.”

Education
- PhD, 2016, Stanford University School of Medicine
- BA, 2008, Molecular Biology, Princeton University
Research Summary
Our bodies are tuned to detect and respond to cues from the outside world and from within through exquisite collaborations between cells. For example, the cells lining our airways communicate with sensory neurons in response to chemical and mechanical signals, and evoke key reflexes such as coughing. This cellular collaboration protects our airways from damage and stabilizes breathing, but can become dysregulated in disease. Despite their vital importance to human health, fundamental questions about how sensory transduction is accomplished at these sites remain unsolved. We use the mammalian airways as a model system to investigate how physiological insults are detected, encoded, and addressed at essential barrier tissues — with the ultimate goal of providing new ways to treat autonomic dysfunction.
Awards
- Warren Alpert Distinguished Scholars Award, 2021
- Life Sciences Research Foundation Fellowship, 2018
